Our Strathfield location has now closed permanently.
For existing follow up and new patient referrals, please see our other Sydney practices:
Dr John Chang
EASTWOOD
www.eastwoodeye.com.au
02 8188 2020
Dr Mark Gorbatov and Dr Kwon Kang
SYDNEY CBD
www.retinavitreous.com.au
02 9223 8880
Diabetic Retinopathy
People with diabetes (type 1 or 2) can develop an eye disease called diabetic retinopathy. A damaged retina can lead to irreversible vision loss and blindness.
High blood sugar levels (over many years) causes damage to the blood vessels in the retina. The damaged blood vessels can leak causing bleeding or block up causing impaired blood circulation and supply of nutrients to the retina, which is vitally important for vision as this is like the “film in the camera”. There are two main stages of diabetic retinopathy.
1. Non-proliferative diabetic retinopathy (NPDR)
This is the early stage of diabetic eye disease and many people with diabetes have it. With NPDR, the damaged blood vessels in the retina leak, resulting in swelling and bleeding of the retina. When the central part of the retina, called the macula swells, it is called “macular oedema”. Macular oedema is the most common reason why people with diabetes lose their vision.
2. Proliferative diabetic retinopathy (PDR)
This is a more advanced stage of diabetic retinopathy and it is less common. PDR is characterised by worsening retinal circulation due to blockage of the damaged retinal blood vessels. When this happens, the retina starts growing abnormal new blood vessels in response. Such abnormal blood vessels are fragile and bleed easily and can lead to development of fibrous scar tissues that pull off the retina (retinal detachment). Both of these complications can lead to blindness.
Often you can have diabetic retinopathy and not know it. This is because it often causes no symptoms (such as eye pain or difficulty seeing) at all in its early stages. This is why it is critically important that all persons with diabetes should have regular periodic screening eye examinations with their eye specialist. Regardless of whether there are any difficulty with vision, all diabetic persons must have their eyes and retina examined so that early diabetic retinopathy is detected and vision loss prevented. As diabetic retinopathy gets worse, it will start causing noticeable problems including blurry vision, difficulty reading, abrupt onset of numerous floaters, or even sudden onset of severe vision loss.
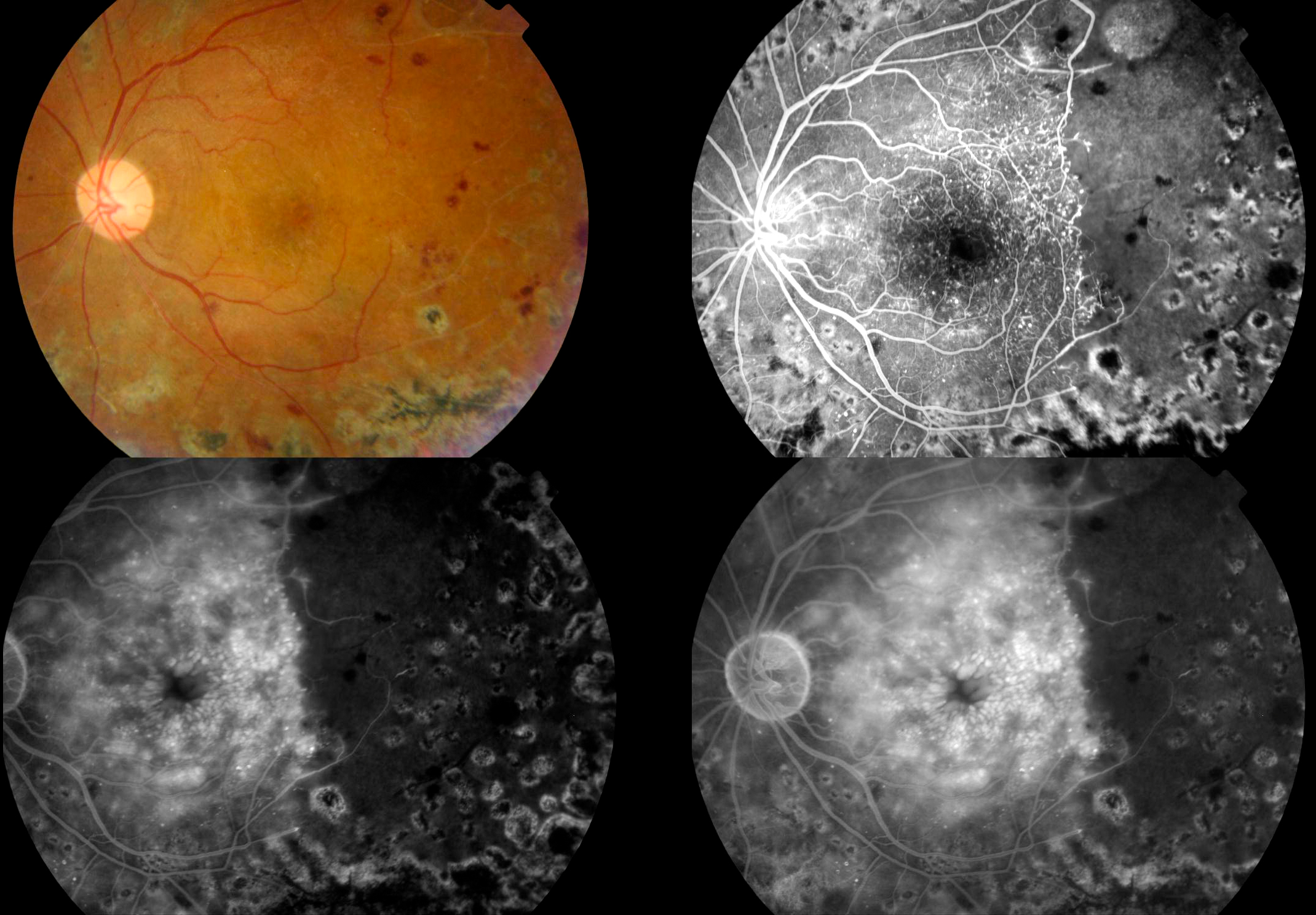
Retinal imaging in a patient with diabetic retinopathy. The first colour photo shows the appearance of the retina as seen by the eye specialist using specialised equipment. Red blotches are bleeds into the retina. The sequence of black and white pictures is retinal angiography, which shows leakage from the damaged retinal blood vessels (white, bright areas) and to the right of this, the darker area represents areas of the retina where there is insufficient blood flow due to the blockage of blood vessels from severe diabetic retinopathy.
Anyone who has diabetes is at risk of developing diabetic eye disease, but the following groups are at higher risk and should be even more careful in ensuring that their eyes are regularly examined:
- Longer duration of diabetes
- Poor blood sugar (high BSL) control
- High blood pressure & high cholesterol
- Cigarette smoking
- Pregnancy
- Other diabetic complications such as poor kidney function, diabetic foot ulcers, peripheral neuropathy
Dr John Chang has been part of an Australian research team that have discovered new genes that places certain people at higher risk of developing diabetic retinopathy and in particular for certain vision-threatening problems due to their diabetic retinopathy. Details of his cutting edge clinical research in this field can be found under the publication list of his biography page.
Diabetic retinopathy is diagnosed by your eye specialist looking through a special lens to see the inside of your eye (retinal examination). To perform a detailed comprehensive retinal examination, dilating eye drops to widen your pupils is necessary.
Specialised retinal imaging tests may also be required depending on the findings, and these include Optical Coherence Tomography (OCT) scans. These use laser light and are quick, comfortable and safe examinations that can be done in the eye specialist clinic during the same visit. OCT scans of the macula may detect early swelling. OCT angiography (OCT-A) allows a high-resolution imaging of the retinal blood vessels without the need for traditional dye injection into a vein.
Treatment of diabetic retinopathy depends on the type and severity of your diabetic retinopathy as well as whether there are vision threatening problems such as swelling of the macula or bleeding abnormal blood vessels. When diabetic retinopathy is mild and vision is unaffected, your eye specialist may not recommend any eye treatment but keep you under ongoing monitoring. Our eye surgeons will tailor the treatment options for your specific circumstances. Broadly speaking, treatment options include:
- Medical control of your blood sugar level (BSL), blood pressure and cholesterol.
- “Anti-VEGF” medication: These help to reduce the swelling of the macula, slowing vision loss and even improving vision. This treatment is given by injections into the eye. This is a very safe and effective treatment that is given in the procedure room of the clinic.
- Retinal laser treatment: Laser therapy might be used to help seal off leaking blood vessels. This can reduce swelling of the retina and this may avoid the need for eye injection treatment or sometimes used in combination with other treatments. Laser treatment can also help shrink abnormal blood vessels in more advanced diabetic retinopathy and prevent them from growing again. Such laser treatment can be comfortably done in Strathfield Eye Surgery.
- Steroid medicine: There is a slow-release steroid implant that can be injected into the eye to treat macula swelling from diabetic retinopathy. One of the key advantages of this treatment is that the slow-release of the medicine means that there is a longer lasting treatment benefit.
- Retinal surgery such as vitrectomy may be required for more advanced diabetic retinopathy causing vision loss from large bleed inside the eye or retinal detachment from scar tissues. Vitreoretinal surgery removes vitreous gel and blood from inside the eye, as well as remove scar tissues from the retina and re-attach it.
Diabetic retinopathy is one of the leading causes of vision loss and blindness in Australia and particularly in younger persons. However, with appropriate treatment, vision loss can be prevented.
- All persons with diabetes (type 1 or 2) must have their eyes examined regularly (at least once a year). Diabetic retinopathy may be found even before you notice any vision problems.
- Ensure that you have good control of your blood sugar level (BSL), blood pressure, and cholesterol. This is managed by your GP and/or diabetes specialist (endocrinologist).
- If you notice any change in the vision in one or both eyes, call your eye specialist without delay.
- Get treatment for diabetic retinopathy as soon as possible. Early treatment before it becomes more advanced in severity is the best way to prevent vision loss.