Our Strathfield location has now closed permanently.
For existing follow up and new patient referrals, please see our other Sydney practices:
Dr John Chang
EASTWOOD
www.eastwoodeye.com.au
02 8188 2020
Dr Mark Gorbatov and Dr Kwon Kang
SYDNEY CBD
www.retinavitreous.com.au
02 9223 8880
Age-related Macular Degeneration (AMD)
Age-related macular degeneration is very common. It is a leading cause of vision loss in people over 50 years of age. Our eye surgeons provide a personalised treatment plan for patients, carefully explaining all the options.
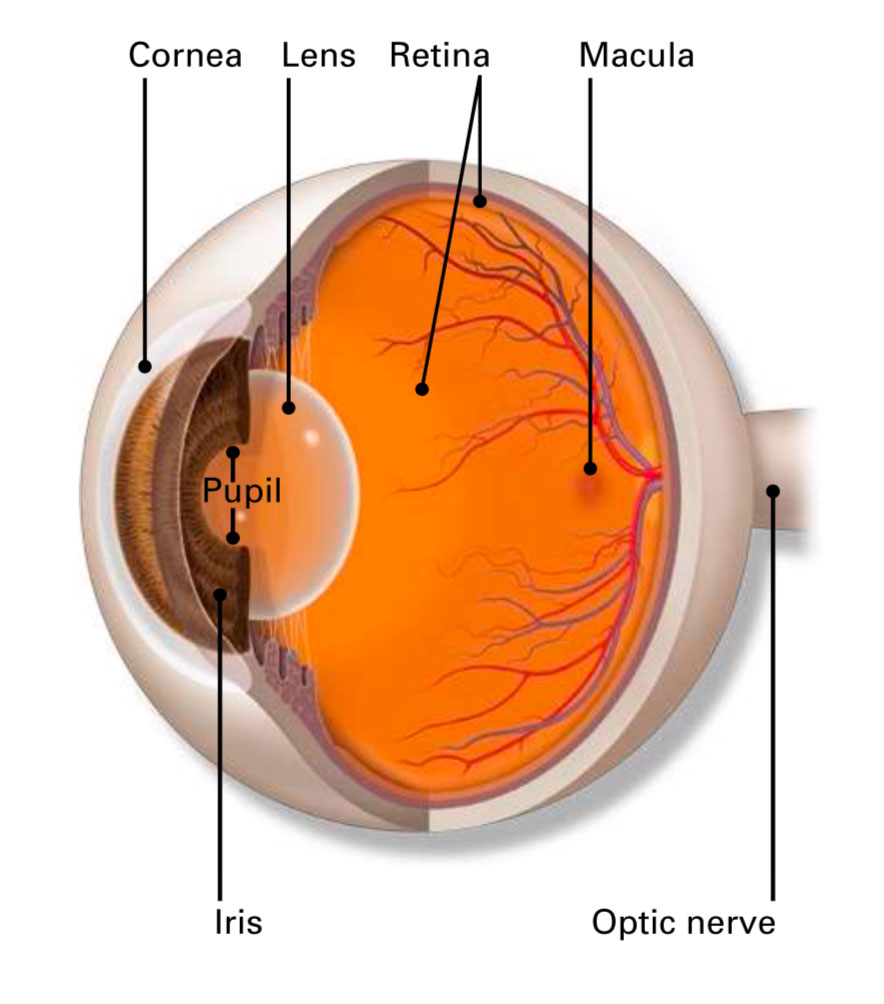
Image from American Academy of Ophthalmology: Cataract Surgery
Age-related macular degeneration (AMD) is a problem with your retina (layer of light-sensitive nerve cells lining the back wall inside the eye, analogous to the film in a camera). It happens when the central part of the retina called the macula is damaged. The macula is the part of the eye that serves your central, high resolution vision, such as reading or recognizing people’s faces. With AMD, you lose your central vision, but your peripheral (side) vision will still be normal.
1) Dry (or atrophic) AMD:
This is the most common type of AMD. In dry AMD, there is “wear and tear” of the macula due to ageing changes and the macula gets thinner (atrophy) with age and tiny clumps of debris called drusen accumulate. There is slow, insidious and progressive loss of central vision with dry AMD. There is no way to treat dry AMD yet but this is an area much medical research.
2) Wet (or neovascular) AMD:
This form is less common but much more serious and aggressive. Wet AMD is characterised by the growth of new, abnormal blood vessels under macula. These blood vessels are fragile and consequently bleed and leak easily, causing swelling of the macula. Wet AMD can present more acutely with central distortion or dark/blurry patch in the central vision. Wet AMD is the treatable form of AMD and hence prompt detection and referral to an ophthalmologist is critical. Without treatment, you lose vision faster with wet AMD than with dry AMD.
It is a common misconception that you can only have either dry or wet AMD. It is not uncommon for patients to have both types of AMD in the one eye, or dry AMD in one eye and wet AMD in their other eye.

With AMD, dark areas may appear in your central vision. This may affect your ability to recognise faces, watch the TV, or to read.
Risk factors for developing AMD include:
- Age over 50 years old
- Family history of AMD
- Cigarette smoking
- Eating a diet high in saturated fats (found in foods like meat, butter and cheese)
- Being overweight
Many people don’t realise that they have AMD until their vision is very blurry. This is why it is important to have regular visits to an eye care professional, especially if you have some of the risk factors above and in particular aged over 50 years. Your eye specialist can look for early signs of AMD before you have any vision problems.
AMD is diagnosed by your eye specialist by a comprehensive eye examination, which includes checking your central vision with visual acuity chart, an Amsler grid, and a retinal examination whereby pupil dilating eye drops are used and your specialist will look inside your eye through a special lens. In addition to detecting the presence of AMD, your doctor can determine what type of AMD you may have as well as its severity and whether any treatment or lifestyle modification is advisable.
Depending on your macula condition, your eye doctor may recommend additional specialized retinal imaging tests including digital retinal photography, OCT macula scan, OCT angiography, fundus autofluorescence, or fluorescein or ICG retinal angiography. These are highly specialised retinal imaging technology and all of these are available at Strathfield Eye Surgery to ensure you receive the most accurate retinal diagnosis and treatment plan.
Dry AMD:
At present, there is no way to treat the dry form of AMD. However, people with lots of drusen or more severe grades of AMD might benefit from taking a certain (AREDS) combination of vitamin supplements. A large study called the AREDS trial found that there is some benefit from taking these vitamins daily to reduce the progression of AMD and vision loss. The specific AREDS vitamin supplementation (daily dosage) consists of: vitamin C (500 mg), vitamin E (400 IU), Zinc (80 mg), Copper (2 mg), Lutein (10 mg), and Zeaxanthin (2 mg). Not everyone benefits from these vitamins. It is best to have yours macula examined and get appropriate personalised advice from your eye specialist.
Wet AMD:
This is the treatable form of AMD and prompt diagnosis and early treatment is very important. Delay in treatment may result in vision loss. The main class of medications used to treat wet AMD are called “anti-VEGF” medications and there are 3 currently available in Australia. This medicine can only be delivered into your eye by an “intravitreal injection” using a very slender (tiny) needle. Naturally, most patients are nervous about such a procedure, but this is really a very safe treatment that can be done very safely in the clinic procedure room. The eye is made numb by eye drops so that there is no pain and the procedure is very quick and you won’t be able to see the needle.
Anti-VEGF eye injections are highly effective in protecting your eye sight from wet AMD and can even result in significant improvement in your vision. These medications help reduce the leakage and bleeding from the abnormal blood vessels that have grown under the macula. Our eye surgeons have performed tens of thousands of intravitreal injections.
AMD causes your central vision to change over time. Early on in its disease course, you may not notice these changes when they happen. But you need to detect such vision changes as soon as possible, rather than until it causes more obvious difficulty with reading for example. This is because treating AMD early can help slow or stop further loss of sight. The Amsler Grid is a useful tool that you can use for self monitoring at home that is simple and quick. A downloadable Amsler Grid is available below. You should use an Amsler Grid every couple of days in the morning, as a habit. It is important to test one eye at a time and to follow the instructions. If you notice that any lines or parts of the grid look wavy, blurry or dim, please contact your eye specialist urgently.
AMSLER GRID
Download PDF.